Mind reveals true extent of crisis in mental healthcare with more than 17,000 reports of serious incidents in past year alone
The UK’s largest mental health charity today publishes previously unseen data laying bare the full scale of the emergency in mental healthcare, with staff reporting 17,340 serious incidents in 12 months.
The Care Quality Commission (CQC) figures shows mental healthcare staff across England reported an incident two times every hour[1] in the last year, where people are treated for issues including self-harm, eating disorders and psychosis.
Incidents included:
-
injuries to patients that caused likely long term sensory, movement or brain damage, or physically damaged their body
-
prolonged physical pain or psychological harm, or shortened life expectancy
-
cases of abuse, including those involving the police
-
injuries for which the patient needed treatment to prevent them dying
The full list of incidents can be found on the CQC website.
The 17,340 serious incidents were reported in hospital, community and residential mental healthcare settings between the beginning of April last year and the same time this year.
 In total:
In total:
-
15,254 reported incidents related to care in private community and hospital settings
-
2,086 related to NHS community and residential places of care
-
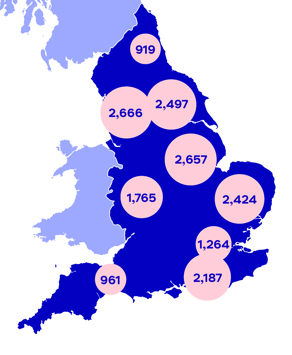
Across all settings, the highest number of reported incidents were in the North West of England (2,666), followed closely by the East Midlands (2,657).[2]
The map above shows how incident reports were spread by region. A full breakdown of the number of incidents by region and type of provider is available.
Many NHS patients receive care in private settings because of pressures on capacity. According to NHS data, approximately 17% of people of all ages who were in contact with secondary mental health services between 2021 and 2022 were seen by a non-NHS provider.[i]
All of these incidents involved care providers raising concerns with the CQC under their statutory duty under Regulation 18.
The previously unpublished data follows a string of abuse scandals in mental health hospitals.
Recent cases include:
-
The Priory Hospital Cheadle Royal near Stockport, in the North West, where Beth Matthews, 26, Lauren Bridges, 20, and Deseree Fitzpatrick, 30, all died between January and March last year.
-
The North East London NHS Foundation Trust (NELFT), where a coroner found that found that a series of failures in care led to the death of 12-year-old Allison Aules last July.
-
The Priory Arnold, in the East Midlands, where a patient died last December after managing to leave the hospital, and another incident this January in which a patient was injured after getting on to its roof.
-
Greater Manchester Mental Health NHS Foundation Trust, where undercover journalists filmed staff using restraint inappropriately and swearing at and slapping patients at the Edenfield Centre in Prestwich last year.
Responding to the data, Dr Sarah Hughes, the Chief Executive of Mind, said:
“It is deeply worrying that healthcare staff across the country are so concerned about the situation in mental health settings that they are reporting a serious incident once every half an hour. We knew this was a crisis – now we know the scale of this crisis. People seek mental healthcare to get well, not to endure harm. Families are being let down by a system that’s supposed to protect their loved ones when they are most sick. The consequences can be and have been fatal.
“Too many people are bearing the brunt of the crisis in mental health services, including those who are powerless within the system because they are detained for treatment. It is clear these failings are systemic. But it does not have to be this way - good mental health hospitals do exist, and people can be given a say in their treatment but proper care must be available across the board.
“It is time to raise the standard. The UK government has the chance to act by passing the Mental Health Bill before the next General Election and prioritising mental health in their political choices and funding decisions. Politicians must not stand by and allow one more person to go through this suffering. They owe it to every family that is picking up the pieces of a broken system.”
Earlier this year, Mind revealed the public’s loss of confidence in mental healthcare, with YouGov polling showing more than 1 in 3 British adults (35%) said they don’t have confidence that a loved one would be safe if they needed hospital mental healthcare.
A third also said they are not confident that a mental health hospital would treat their loved one with respect (32%) or compassion (34%).[ii]
Join the fight to raise the standard of mental health hospitals.
Notes to editors
-
NHS England is running an inpatient quality improvement programme with £36million government funding.
-
You can find out more about Mind’s Raise the Standard inpatient campaign on our website.
[1] 1.9 times an hour between 1 April 2022 and 31 March 2023.
[2] The number of notifications may vary between providers depending upon the number and demographics of the people to whom they provide services, the type of services provided and other factors. More than one provider might also notify the CQC of the same incident.
[i] Mental Health Bulletin, 2021-22 Annual report. Of 97,160 people of all ages who were in contact with NHS funded secondary mental health, learning disability and autism services and admitted in 21/22, 16,841 were admitted to non-NHS provider.
[ii] Figures are from YouGov Plc. Total sample size was 2,014 adults. Fieldwork was undertaken between 7th - 8th June 2023. The survey was carried out online. The figures have been weighted and are representative of all GB adults (aged 18+).











